80y/o with Shortness of breath
CBBLE UDHC Similar cases
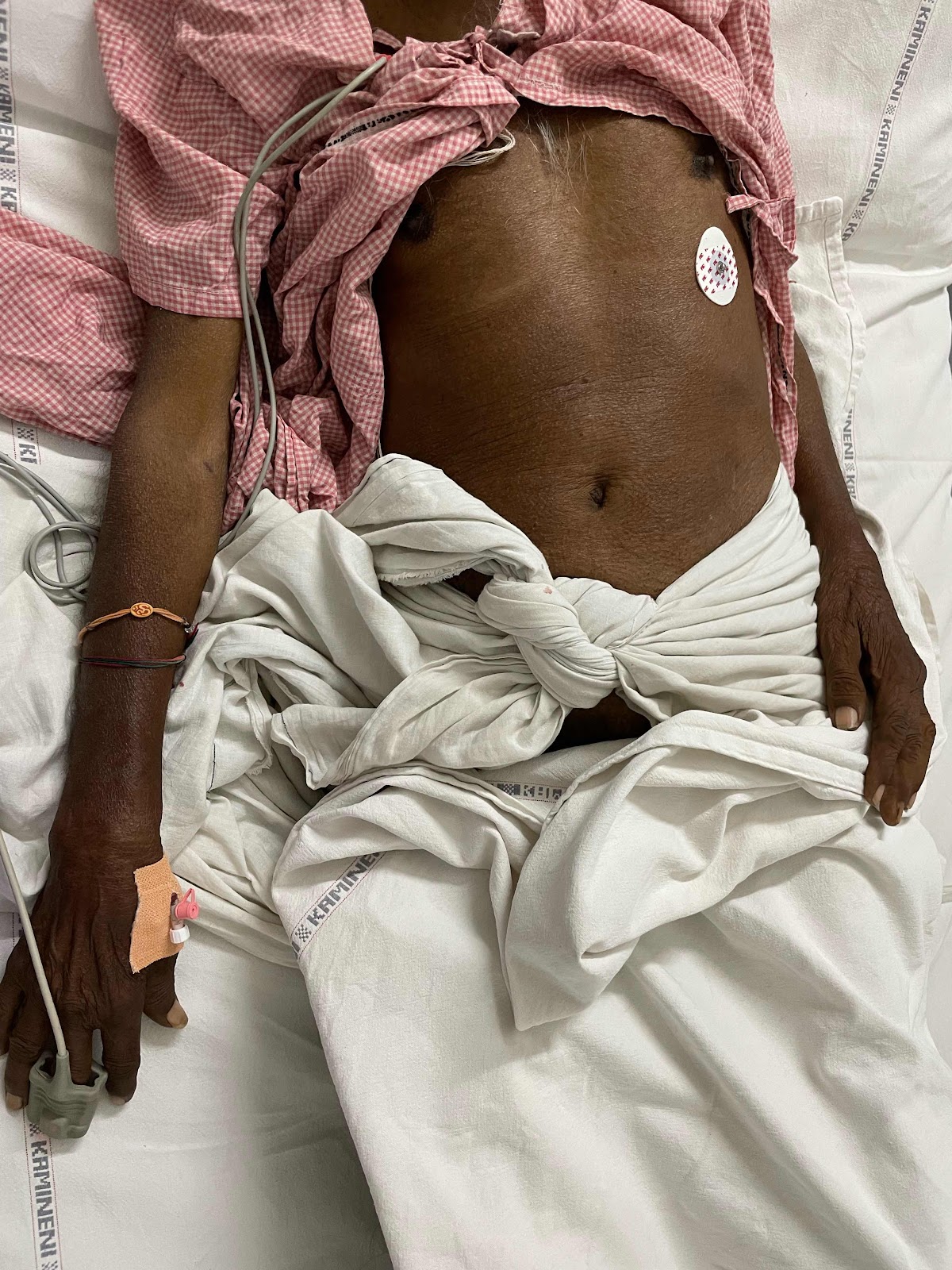

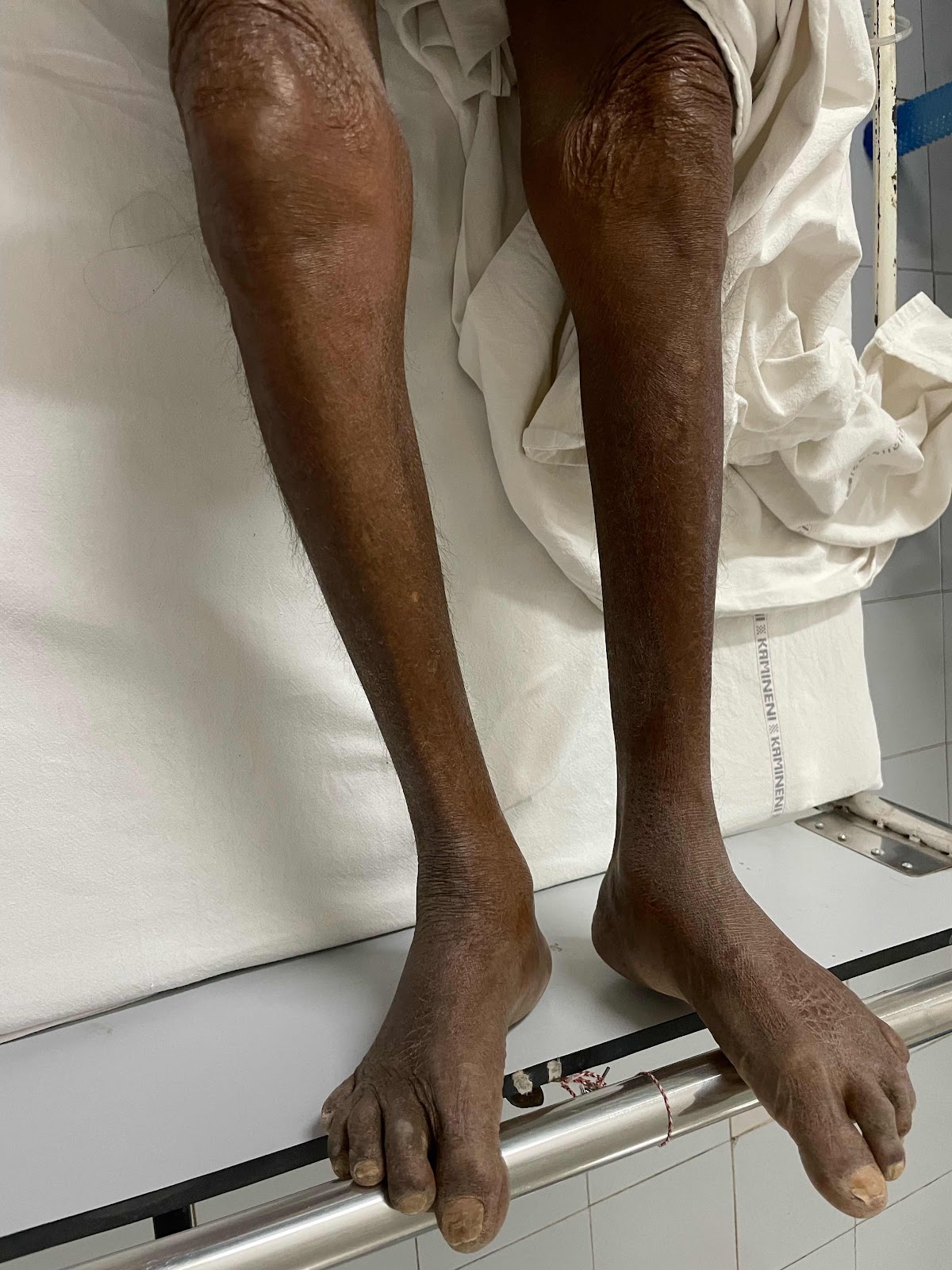
Investigations:

ECG

BGT: B positive
This is an online E log book to discuss our patient's de-identified health data shared after taking his/her/guardian's signed informed consent. Here we discuss our individual patient's problems through series of inputs from available global online community of experts with an aim to solve those patient's clinical problems with collective current best evidence based inputs. This E log book also reflects my patient-centered online learning portfolio and your valuable inputs on the comment box.
An 80 year old male, weaver by occupation(until 5 years back), came to the casuality with:
- Complaints of sudden worsening of Shortness of breath at 7pm on 8/3/22, present since 10days.
Patient was apparently asymptomatic 10 days back and then he developed Shortness of breath grade II, which was insidious in onset, not associated with Orthopnea or paroxysmal nocturnal dyspnea. It was relieved on taking bronchodilators.
From 7:00pm, patient developed sudden onset of Shortness of Breath (grade IV) and was brought to our hospital. He stopped taking bronchodilators 2 days back.
No history of fever, chest pain, palpitations or pedal edema.
Past history:
No Diagnosis of DM, HTN, TB or epilepsy was made.
Treatment history:
- Ipratropium bromide and Levosalbutamol 200 MDI
- Tab. Theophylline (23mg) and Etophylline (77mg) BD
- TAB. Montec(10mg) LC (5mg)OD
General examination:
Patient is conscious and coherent.
No pallor, icterus, clubbing, cyanosis, lymphadenopathy or pedal edema.
Vitals on admission:
Temp: 98.5
PR: 119 bpm
BP: 170/100 mm hg
RR: 41
GRBS: 159 mg/ dl
CVS: S1 S2 PRESENT
RS: BAE +
Inspiratory wheeze present in inframammary, infra axillary and infra scapular area. R> L
CNS: NAD
P/A: soft
Investigations:
ABG:
At 1:51 AM
pH: 7.21
pCO2: 25.2
pO2: 89
HCO3: 9.8
At 5:46 AM
pH: 7.311
pCO2: 24.2
pO2: 190
HCO3: 14.5
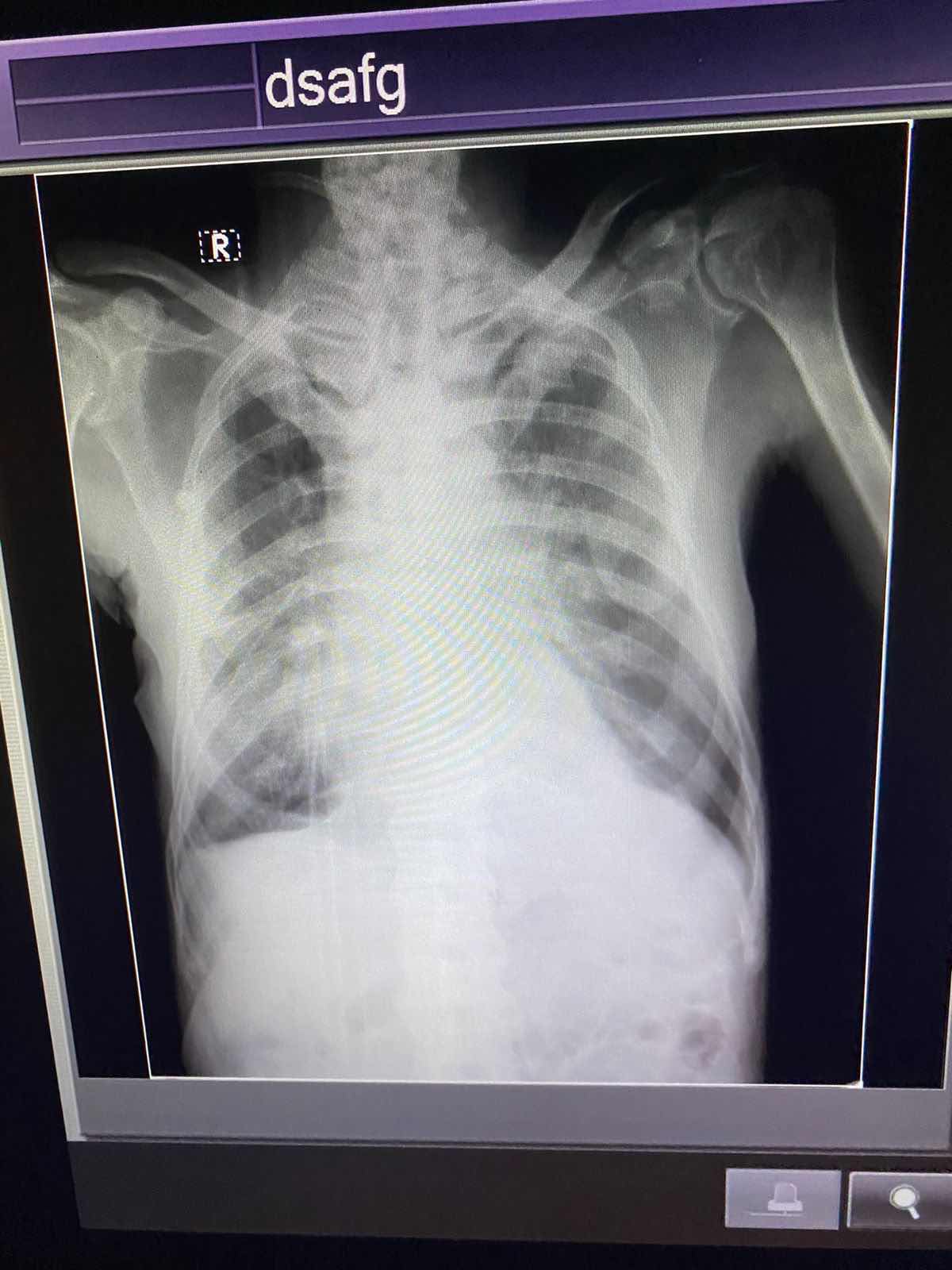
Chest X ray
On 26/2/22
On 9/3/22
ECG
BGT: B positive
Diagnosis: ?Acute pulmonary edema secondary to heart failure secondary to hypertensive emergency
?A/E of COPD
Metabolic acidosis
Treatment:
- Head end elevation.
- Inj. LASIX 40mg IV TID
- Nebulization with Ipratropium and budecort every 6th hourly.
- O2 inhalation to manautiyan SpO2 >90%
- Vitals monitoring
- Strict I/O charting
AP diameter of chest= 21cm
Lateral diameter of chest= 18cm
10/3/2022
NEW ADMISSION
AMC BED NO/1
S:
Shortness of breath decreased compared to yesterday
O:
Patient is conscious, coherent and cooperative
Pallor present
No icterus, cyanosis, lymphadenopathy or pedal edema.
BP: 110/80 mmhg
PR: 76BPM
RR: 22
GRBS: 160 mg/dl
CVS: S1 S2 Present, no murmurs
RS:
Wheeze heard in infra mammary area, infra axillary area and infra scapular area.
Position of trachea: central
Vesicular breath sounds heard.
CNS: E4V5M6
A:chronic renal failure
Acute exacerbation of copd
P:
1.Head end elevation.
2. Inj. LASIX 40mg IV TID
3.Nebulization with Ipratropium and budecort every 6th hourly.
4.O2 inhalation to manautiyan SpO2 >90%
5.Vitals monitoring
6.Strict I/O charting





Comments
Post a Comment